No kidding!
[Childhood cancers are highly curable]
A child is not a small adult.
That a maxim drilled into students of paediatrics in medical schools.
“Everything, right from diagnosis to treatment, is entirely different for a child in comparison with the same disease in an adult,” says Dr Shripad D. Banavali, director, academics, Tata Memorial Centre, Mumbai. “In India, if there are a hundred cases of cancer, three to four of them will be childhood cancers as against one or two in the developed world. This is because we have a higher number of children, given our population.”
While cancers in adults are preventable and controllable, in children they are unpreventable but highly curable, say doctors. For example, as Banavali puts it, in a sample of 100 children with cancers, the cure rate is 80-85 per cent. In the age group of 0-18 years, 50 per cent of children with cancer diagnosed with blood cancer or leukaemia and the rest have solid tumours. Within solid tumours, which can affect any organ, the commonest ones are brain tumours.
If the fever does not subside, then along with a complete blood count, the parent or the doctor has to request the pathologist to check for leukaemia. —Dr Shripad D. Banavali, director, academics, Tata Memorial Centre, Mumbai We are looking at risk-certified therapy, which means giving intensive treatment for high-risk cancer and little treatment for low-risk cancers—Dr C.P. Raghuram, consultant, paediatrics, haematology and oncology, Aster CMI hospital, Bengaluru.
“If a child does well for five years post-diagnosis, we say that he or she is cured of cancer. Other problems may persist, but they would be cured of cancer,” says Banavali. “This is because there are high chances of relapse in adults, but not in the case of children. Once cured, it is very rare that a child suffers a relapse later in life. ”Now the challenge before experts is to not just cure the child of cancer but to ensure they lead fuller lives. “Earlier, we only bothered about survival because that in itself was a challenge,” says Banavali. “But now, as we progress, we are over that phase. Our success rates are good and now we want to make these children healthy enough to lead fuller lives as adults, without any problems.”
This is why doctors now stick to treatments with the lowest risk. Most cancers of the blood in children do not require radiation and have a tailored treatment protocol, which does not lead to harmful long-term side effects. Radiation is opted for only in high-risk cases or cases where the tumours have grown too big and the cancer is at a later stage. “For childhood cancer to be completely treatable, the diagnosis has to be very early and proper,” says Dr C.P. Raghuram, consultant, paediatrics, haematology and oncology, Aster CMI hospital, Bengaluru. “With advancements in technology, we are now able to identify not just the main type of lymphoma but even its sub-types and treatments have become super-specialised. We are not just looking at curing paediatric cancers, rather. We are looking at risk-certified therapy, which means giving intensive treatment for high-risk cancer and little treatment for low-risk cancers.”
Childhood cancer is a systemic disease, say, doctors, which means that by the time it is diagnosed, cancer has already metastasised to an extent. There has now been a shift in treatment. Instead of performing surgery before chemotherapy, doctors are doing the reverse. A typical treatment plan involves chemotherapy followed by surgery and, if necessary, radiation. This has changed outcomes—from earlier 10-20 per cent cure rate to now more than 80 per cent, explains Banavali. This way the body is sterilised and the tumour or the disease is not present in different corners. This is also termed neoadjuvant treatment.
The symptoms of paediatric cancers are not different from those of other ailments, such as fever, joint pain and headache. However, these symptoms in a normal child will subside within three to five days but not so quickly in a child with cancer. And, that is the first sign that something is serious, says paediatric haematoma-oncologist Dr Gaurav Kharya. In children with persisting headache and vomiting, the most ideal thing to do is get an MRI, not a CT scan, of the brain. “If the fever does not subside, then along with a complete blood count. The parent or the doctor has to request the pathologist to check for leukaemia,” says Banavali.
“Because now everything is so automated, lab technicians and pathologists do not check a sample under the microscope. Hence, please request them to do it.” Banavali recounts how he has seen patients who had been misdiagnosed and put on anti-TB medication for six months. “And then they come to us with enlarged tumours,” he says. “If a parent observes that medicine is not working, stop it immediately and suspect something more serious. In children, biopsies provide the most accurate results for proper diagnosis.”

Experts believe that cancer treatment outcome in major centres is close to 75 per cent, but overall in India, it is around 40 per cent only. It is still not very common to have paediatric cancer units in hospitals. In India, because it is highly labour-intensive and cost-intensive, say doctors. Behind each patient in a hospital’s paediatric oncology unit, there is a team of at least 20 people, including an oncologist, surgeon, radiotherapist, radiologist, surgical pathologist, molecular biologist, anaesthetist, palliative care specialist, psychologist, nursing team, nutritionist and social worker. “This means one patient as against 20 specialists. This makes it very, very labour-intensive and a highly expensive proposition for a hospital to invest in paediatric cancer”.
“It literally requires a village to treat a child with cancer,” says Banavali. Also, every year, 35,000 to 40,000 children are diagnosed with cancer as against 10 lakh to 12 lakh adults, he adds. That is too high an investment for a smaller number of patients. “Yet, we ask the government to invest in infrastructure. If [it is] not increasing the number of centres, at least make those that are already functioning self-sufficient. At present, not every major city has even one fully developed paediatric cancer unit,” says Banavali. The Tata Memorial Hospital treats more than 3,000 children with cancer a year, which, says Banavali. Is three times the children treated across the 40 specialised centres in the UK.
Sahara Shah, 17, Leukaemia

The credit for her “incredible treatment and recovery”, she says, goes to her mother Shanti. Her mother left her hometown in Nepal the day Sahara was diagnosed and came. To Mumbai’s Tata Memorial Hospital with barely 01 lakh and an identity card. Shanti had to make that journey alone as her husband. Who worked in the Middle East, had gone missing around the same time. “It was the mother’s persistence that has paid off,” says Banavali. I am perfectly healthy and fine and have never really felt like it.
A cancer survivor because I never felt sick at all. —Sahara ShahShanti would travel close to 100km from Ambernath to Mumbai and back for Sahara’s chemotherapy sessions. “It started with a mild but persistent fever, and the doctors kept misdiagnosing,” says Shanti. A biopsy concluded that Sahara had acute lymphocytic leukaemia (ALL), a cancer of the blood and bone marrow. The disease progresses very fast and creates immature blood cells rather than mature ones. A cell’s DNA contains a working manual, with instructions.
Banavali says that Sahara was a low-risk patient as she came in time for treatment. She underwent chemotherapy cycles for six months on alternate days, and thereafter oral chemotherapy for two and a half years. “Post that, she took a vaccine once a month for nine months and since. Then she goes to a hospital for regular checkups as a cancer survivor,” says Shanti. Who works as a counsellor for parents of children with cancer at Sion hospital.

On November 16th, ultrasound and CT scan revealed a swelling. In the pancreas, and the specialist diagnosed it as pancreatitis (inflamed pancreas). The treatment involved taking two injections every day. But the pain persisted. He is a fantastic football player and sprinter and gets full marks in his studies, too. —Dinkar Sharma, Rudransh’s father. Rudransh was then taken to Medanta-The Medicity in Gurugram. Gastroenterologist Dr Ranbeer Sood suggested that Rudransh be admitted immediately and he ordered an MRI and biopsy. That is when they found that Rudransh was suffering from lymphoma, cancer.
In the body’s infection-fighting cells of the immune system called lymphocytes are present in the lymph nodes, spleen, thymus, bone marrow and other parts. In lymphoma, these lymphocytes change and grow. “At a very, very rapid rate, so much so that they double up in every 24 hours”, says Kharya who treated Rudransh. “The diagnosis of cancer had left us shocked and shaken,” says Rudransh’s father Dinkar Sharma. A London School of Economics graduate who works with a leading government bank in Alwar, Rajasthan. “The doctors began talking about 10-year survival rates, which was too disturbing and frightening”. We lost our sleep and appetite. I remember how my wife and I would cry, fearing we might lose our son.
We consulted Ayurveda, homoeopathy and what not to see if his cancer could be cured. We even took to palmistry and would read his palm. While he was asleep to check if he had a long lifespan. Did does not tell him that he had cancer. Just that he needs to take proper medication for his tumour to go away. The PET scan, says Dinkar, revealed that the tumour, an 8cmx3cm oval-shaped ball, was in the abdomen. It was big enough to suppress other organs, including the diaphragm and lungs. His cancer, fortunately, had not spread to other organs. “At the time we saw Rudransh, the disease was taking over him progressively,” says Kharya. “He had lost almost 12kg in a month, was not able to eat well, had abdominal pain and distension, nausea and vomiting.”
Rudransh, says Kharya, wrongly received partial treatment for intestinal tuberculosis, before a biopsy confirmed it to be Burkitt lymphoma. “It is a form of non-Hodgkins lymphoma in which cancer starts in the immune cells called B-cells,” he says. “It is associated with impaired immunity and is rapidly fatal if left untreated. He was at the intermediate stage when he was brought to us, but the disease burden was huge. He was fed through a tube initially and then he was given two cycles of chemotherapy.”
After the second cycle, Rudransh’s symptoms resolved significantly; the abdominal lump disappeared and his appetite improved. To date, Rudransh has received five cycles of chemo. He would need two more cycles to complete the treatment. But the side effects of chemo were unbearable. Even though they were considerably reduced by drinking almost seven litres of water every day. “He had acute pain in the jaw, so much so that at times he could not even. Drink water but then he persisted,” recalls Dinkar. Burkitt lymphoma, if treated aggressively, can have a very good outcome, explains Karya.
The success rate for stage one and stage two Burkitt lymphoma is more. Then 95 per cent and 80-85 per cent for stage three. So, early detection and treatment are the keys to cure. When Dinkar noticed that his son was perspiring profusely at night, causing bedsheets and his clothes to turn damp. Suffering from a loss of appetite with frequent vomiting and intense abdominal pain, he wasted no time in consulting doctors.
“It was only later that we learnt the cause behind frequent vomiting. The food was unable to pass from the stomach into the intestines because of the tumour,” said Dinkar. At present, Rudransh, who will soon be in class eight, weighs 35kg, has more alkaline food. Does his daily pranayams and attends his online classes regularly. “He is a fantastic football player and sprinter and gets full marks in studies, too,” says Dinkar. “We cannot wait to finish the treatment so that Rudransh can come out. The shadow of cancer and walk into the sun, hale and hearty.”
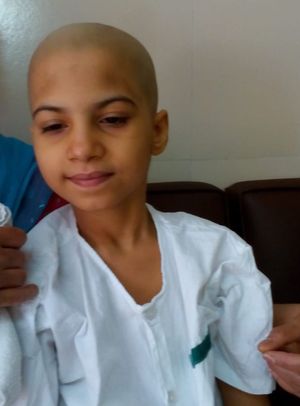
Samira Haryan, 14, Brain tumour
Samira all often when she diagnosed with a brain tumour in 2017. Four years later, the fear of relapse still looms large in the Haryan household. Every time Samira complains of headache, her father Deepak Haryan wonders. If “it has come back to haunt the family again”. Samira, says Deepak, had always a healthy child. She would eat, play, study and do all the things that normal kids her age would do. The problem began when she started getting irritated with the tube light flickering in the house. She also showed signs of fatigue and drowsiness.
“We thought she needed spectacles, but the optometrist found that her entire optic nerve had turned. Red and asked us to immediately see an eye specialist. The latter, in turn, suggested an MRI, which pointed to a brain tumour.” Samira’s tumour surgically removed. “Things were normal for a few days, but soon the problems resurfaced,” recalls Deepak. Six months after the surgery, Samira began to vomit frequently and “her eyes showed. A pale white film that was very disturbing to see,” says Deepak. Also, her pupils would dilate on their own at times. A CT scan showed an accumulation of water in the part of her brain where the tumour once resided.
Medically, it called hydrocephalus—the build-up of cerebrospinal fluid. In the cavities of the brain, thereby causing increased pressure inside the skull. It leads to headaches, double vision and poor balance. This necessitated the surgical placement of a hollow tube or shunt inside the brain to help drain. The fluid and redirect it to another location in the body where it could be reabsorbed. However, in another six months, the symptoms came back. “Frequent vomiting, profuse sweating and seizures became a part of Samira’s life. Sometimes it seemed as though she had no life inside of her; she looked so pale and weak,” says Deepak. She has dreadful thoughts of hospital visits and MRI scans.
She considers herself to be a sick child and hates herself for it. —Deepak Haryan, Samira’s father another MRI done, this time at Mumbai’s Jaslok hospital under the supervision of Dr Sudheer Ambekar, a neurosurgeon. “The MRI showed that the shunt had migrated from its original position. That was causing a fluid accumulation in the brain. Which can eventually lead to death if not treated in time,” says Ambekar. “The cause for the dislocation not known and unless it gets infected. The shunt does not have to be replaced.”
Another surgery is done to relocate the shunt to its original position. As of now, Samira is back to normal, except for “a lasting weakness. In limbs and a slight physical imbalance which requires her to held when crossing the roads”. She excels at her studies. While she cannot take up outdoor sports because of her health, she does enjoy indoor games. She is playful and chatty but has grown fearful in the past few years, says Deepak. “The slightest of headaches drives her into a tizzy,” he says.
“She has dreadful thoughts of hospital visits and MRI scans. She considers herself to a sick child and hates herself for it”. Post the last surgery, she has had no complaints. “Yet we prepared for any emergency because going by our experience, issues seen after long gaps of time,” says Deepak. The next MRI is due in May; the last one has done a year and a half ago. “She has to test on a regular basis,” says Ambekar. “Every two to three years, she will have to get. An MRI has done to observe if the shunt in its right place.”
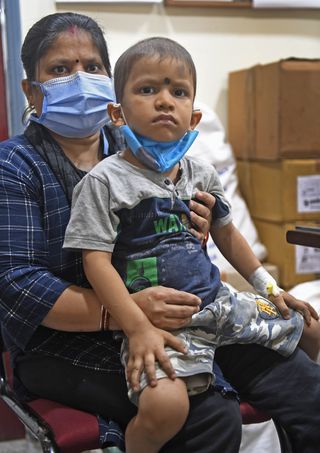
Arnav Tiwari, 4, Blood Cancer
Last August, Arnav Tiwari, 4, brought to Mumbai from Shahdol in Madhya Pradesh for treatment of blood cancer. “He just kept getting a mild fever on and off and was losing weight at a rapid pace,” says his mother. “Doctors there diagnosed him with infections. But when his haemoglobin levels fell below three, they sensed something wrong. We were then referred to Tata hospital, where he diagnosed with leukaemia.”
The family has been staying in Mumbai for the last six months under the care provided by Tata’s Impact Foundation. Arnav has undergone three chemotherapy cycles till now and has one more to go. The little boy playfully jumps into his mother’s lap and nudges her to play with him. His eyes twinkle each time he has spoken to. He listens carefully to the interview and volunteers to narrate little anecdotes. Two months ago, Arnav caught Covid-19. His mother and father, who works in a shop in Shahdol, however, tested negative. Arnav has now tested negative, too.
“Previously, we were also unaware as to what Covid-19 would do in cancer patients,” says paediatric oncologist Dr Girish Chinnaswamy. “We were admitting and isolating them, and delaying chemotherapy. But then we learnt that delaying chemo would be wrong. If in a week’s time, they showed no major problems, we would start the chemo in the Covid-19 ward itself. Many patients were treated this way because cancer is more dangerous. Then Covid-19 and we cannot afford to let the disease relapse.”

Shubham Kumar Prajapat, one-and-a-half years Retinoblastoma
This Magazine(Health Plus) No kidding! appeared first on theweek.in.




